It took six years to be ready to share the images below of my baby. My son. Why now? Almost six years after I stopped using topical steroid creams on his skin. Three years after he rebounded to oral and inhaled steroids while hospitalized for an acute respiratory issue. Why? Because my son is a recovery story to join the thousands of babies, kids, and adults who should never know this preventable condition. How can so many more, thousands of individuals and parent caregivers, still be suffering years later? Their stories posted in Topical Steroid Withdrawal support groups on Facebook and Reddit are not reaching mainstream medicine as the epidemic they represent.
If you know someone dealing with unexplainable, uncontrolled eczema and it worsens each time they attempt to cease or taper using topical steroid creams, they too may be experiencing topical steroid addiction and withdrawal due to the effects of topical corticosteroids when not administered safely. Learn more at ITSAN.org


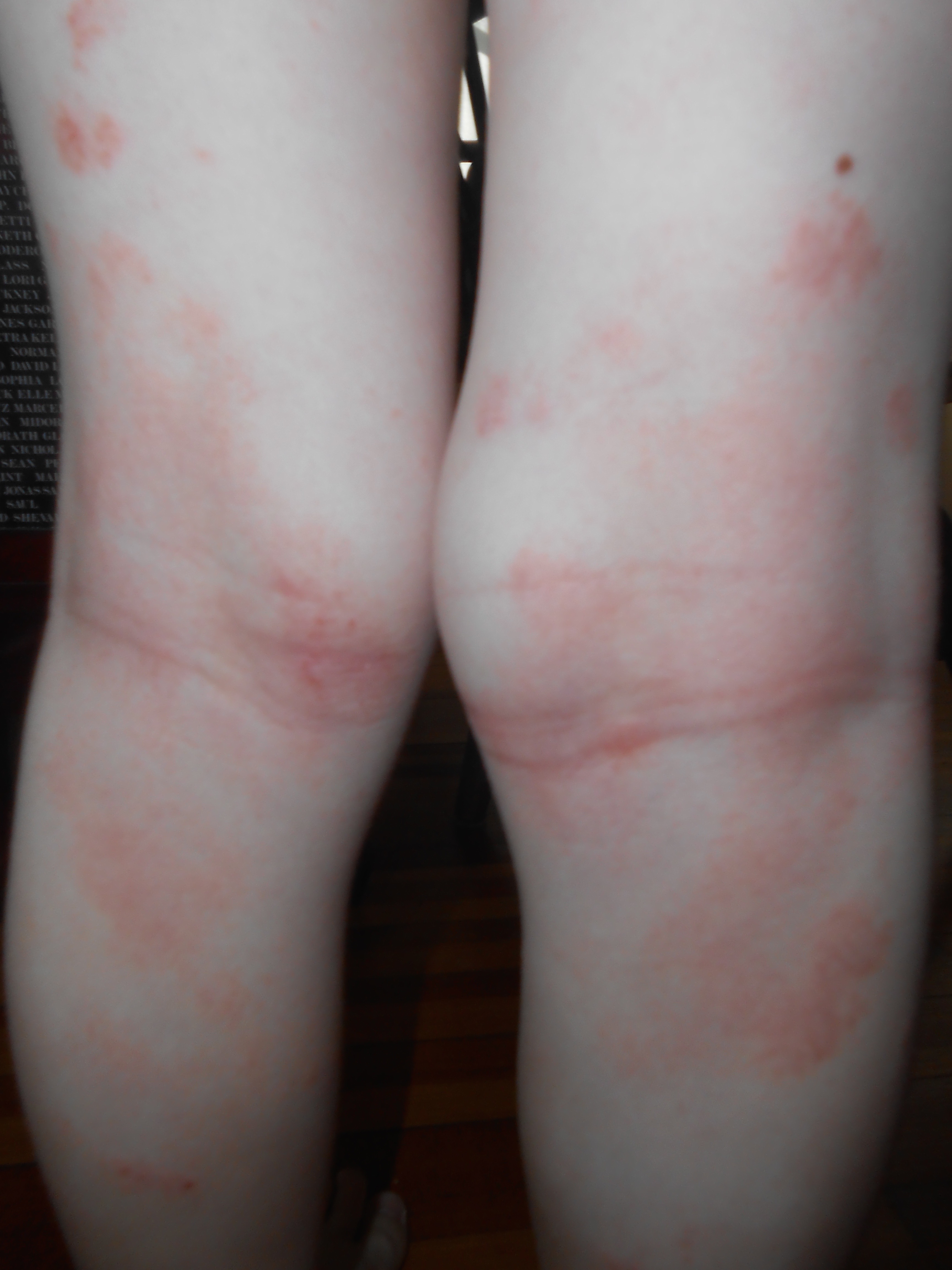


March 2014 (4 yr 4 mo) – Throughout the years that I followed instructions to treat my son Max’s rashes with topical steroid creams (originally just in creases/skin folds such as behind knees or inside elbows), as the rashes would improve and I would reduce the steroid creams as instructed by his pediatrician, his body would react with new rashes. At age four years, his rashes began to spread (pictured above), and I believed that the steroid creams were not helping and making his skin condition worse. I informed his pediatrician of this concern during an office visit in March 2014. In May, I repeated my concern with the same pediatrician and she had an expression on her face that looked like anger. She said “he has maxed out my scope of care.” Max was 4 years 6 months old and had been prescribed topical steroid creams (used intermittently), for close to four and a half years.

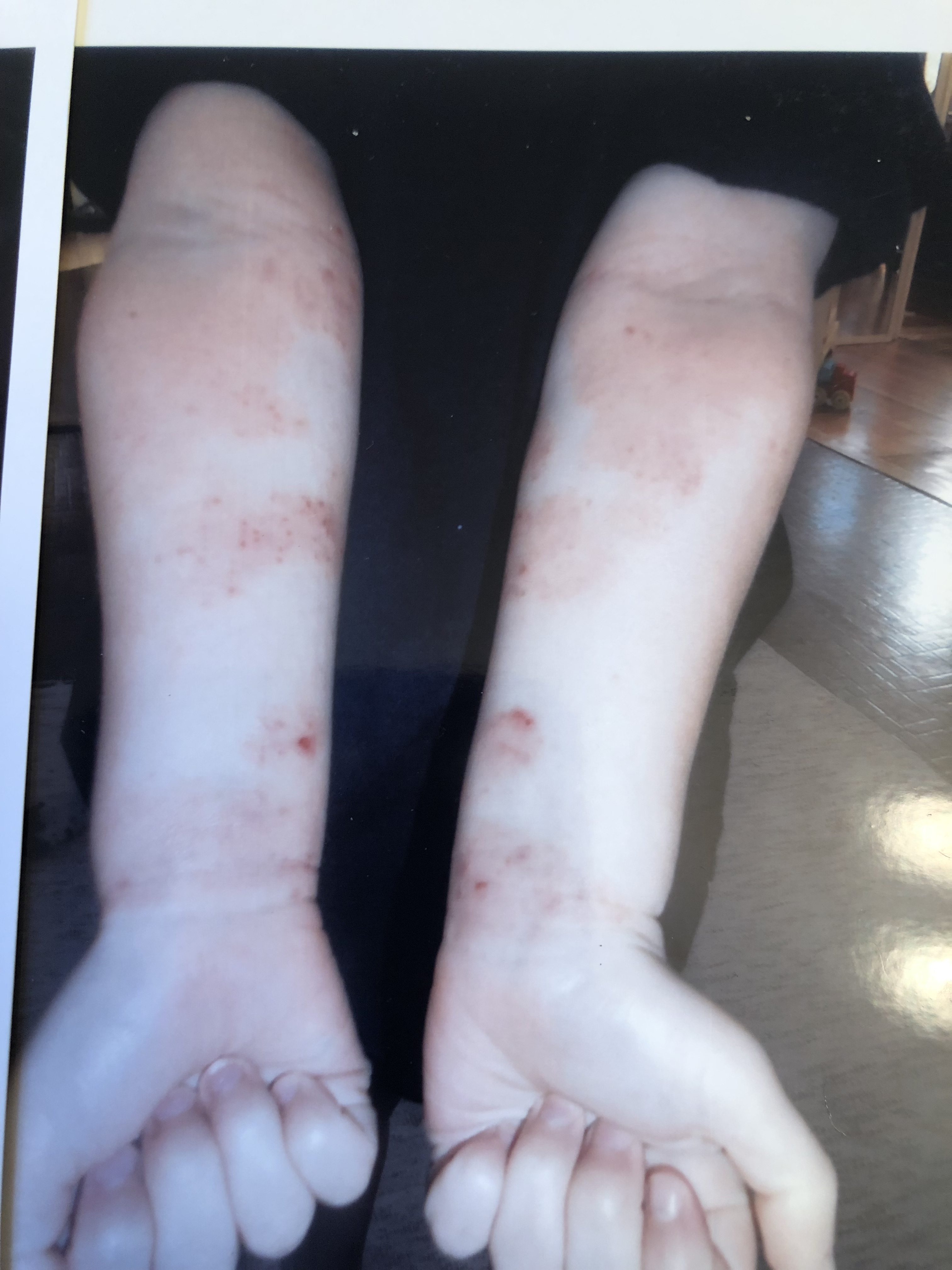
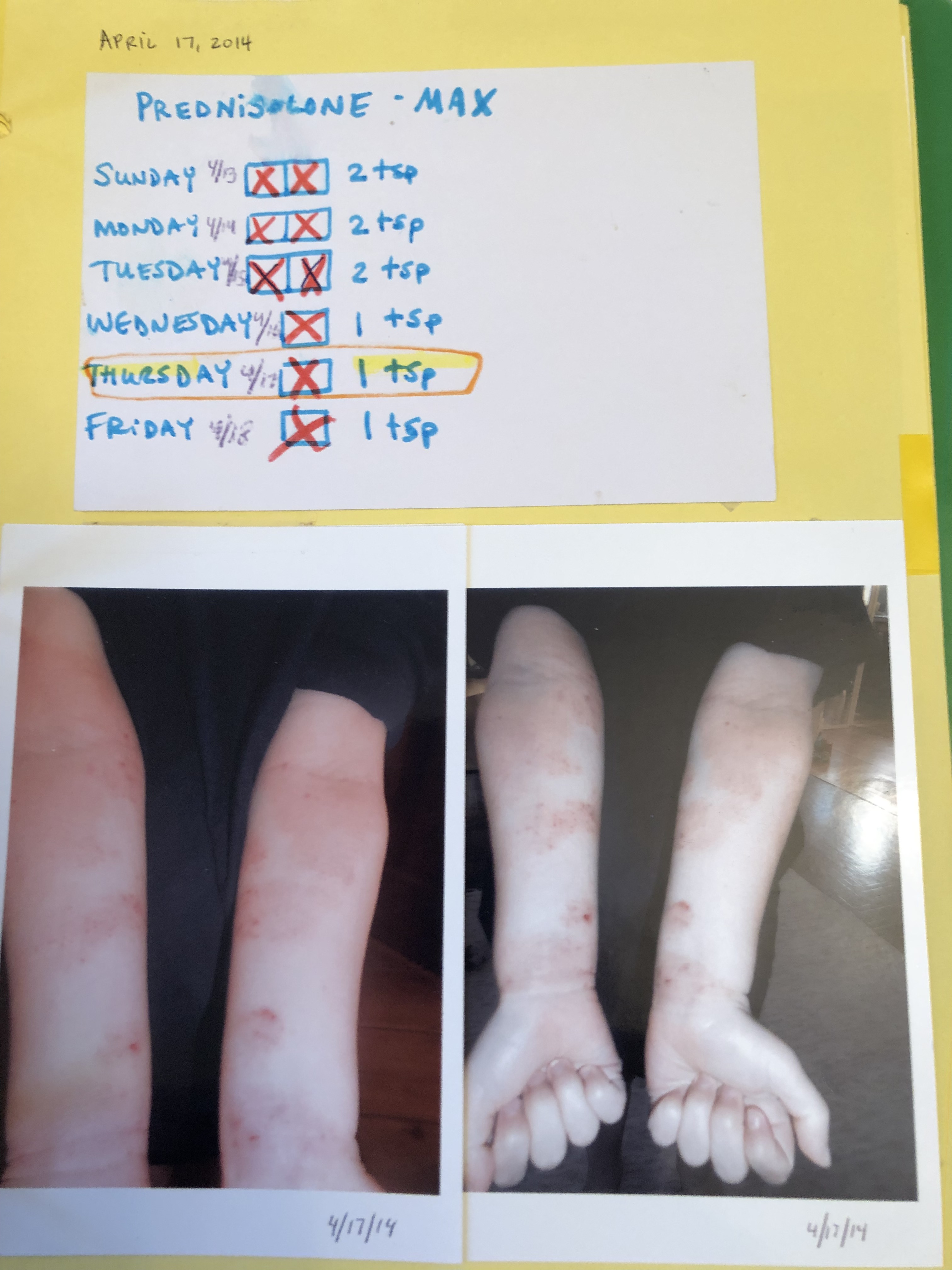
April 2014 (4 yr 5 mo) – Max stopped sleeping at night in mid April 2014, due to the discomfort of his rashes. He was seen on a weekend at an urgent care facility and prescribed a 6 day course of an oral steroid. The medicine only suppressed his rashes for a short time. Seen above on his 5th day on the oral steroid.

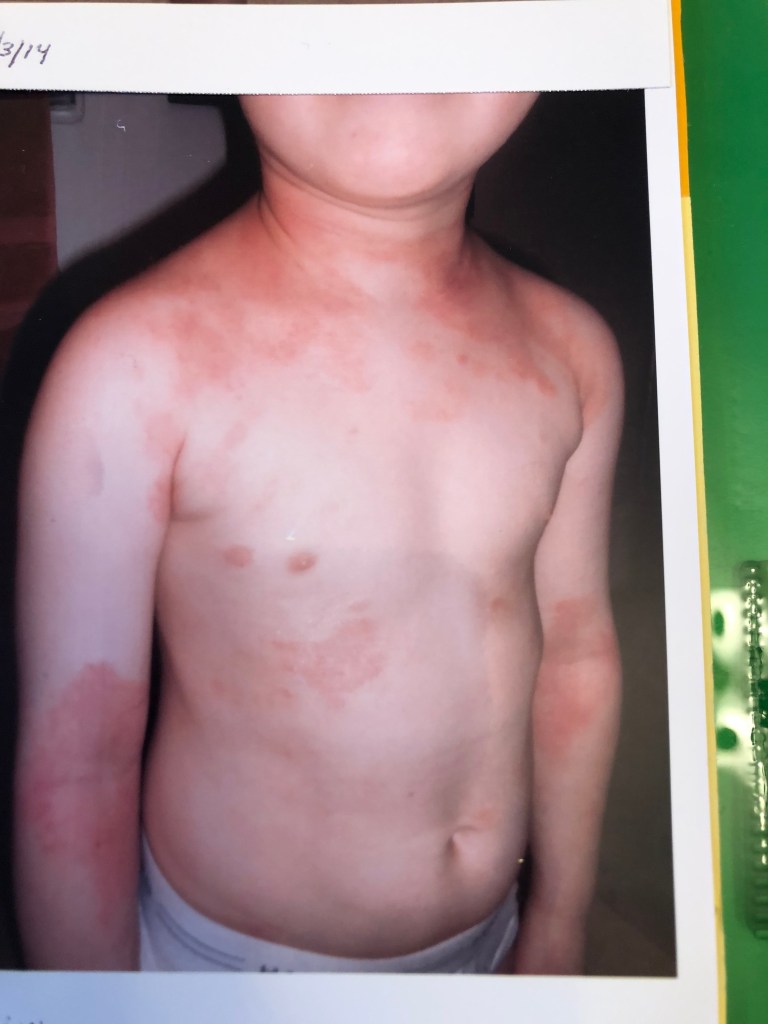
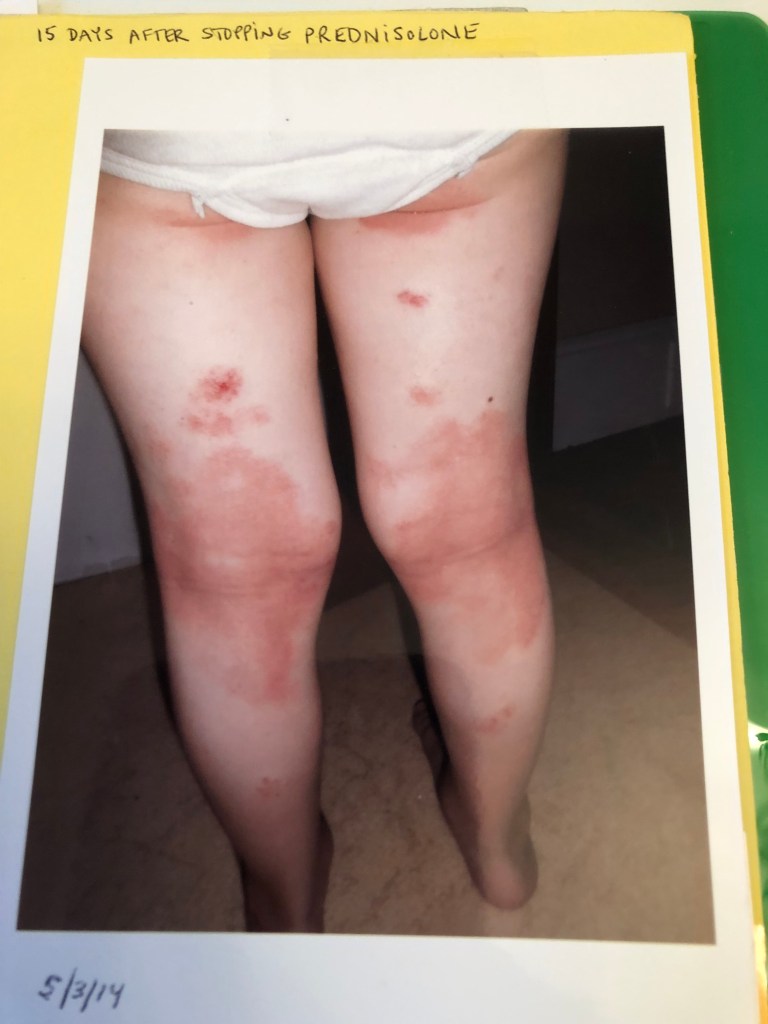
May 2014 (4 yr 6 mo) – At 15 days off the 6 day course of oral steroid, Max’s skin flared with rebound rashes. Max’s pediatrician recommended a 16 day dose (with taper), of an oral steroid. Afterwards Max became highly reactive to multiple environmental allergens. He could not walk across grass without tearing at his legs due to severe itch. We couldn’t go in stores as he reacted to fragrance with terrible arm and leg itch. An allergist tried to convince me to put Max on an immunosuppressant, I researched it and refused.
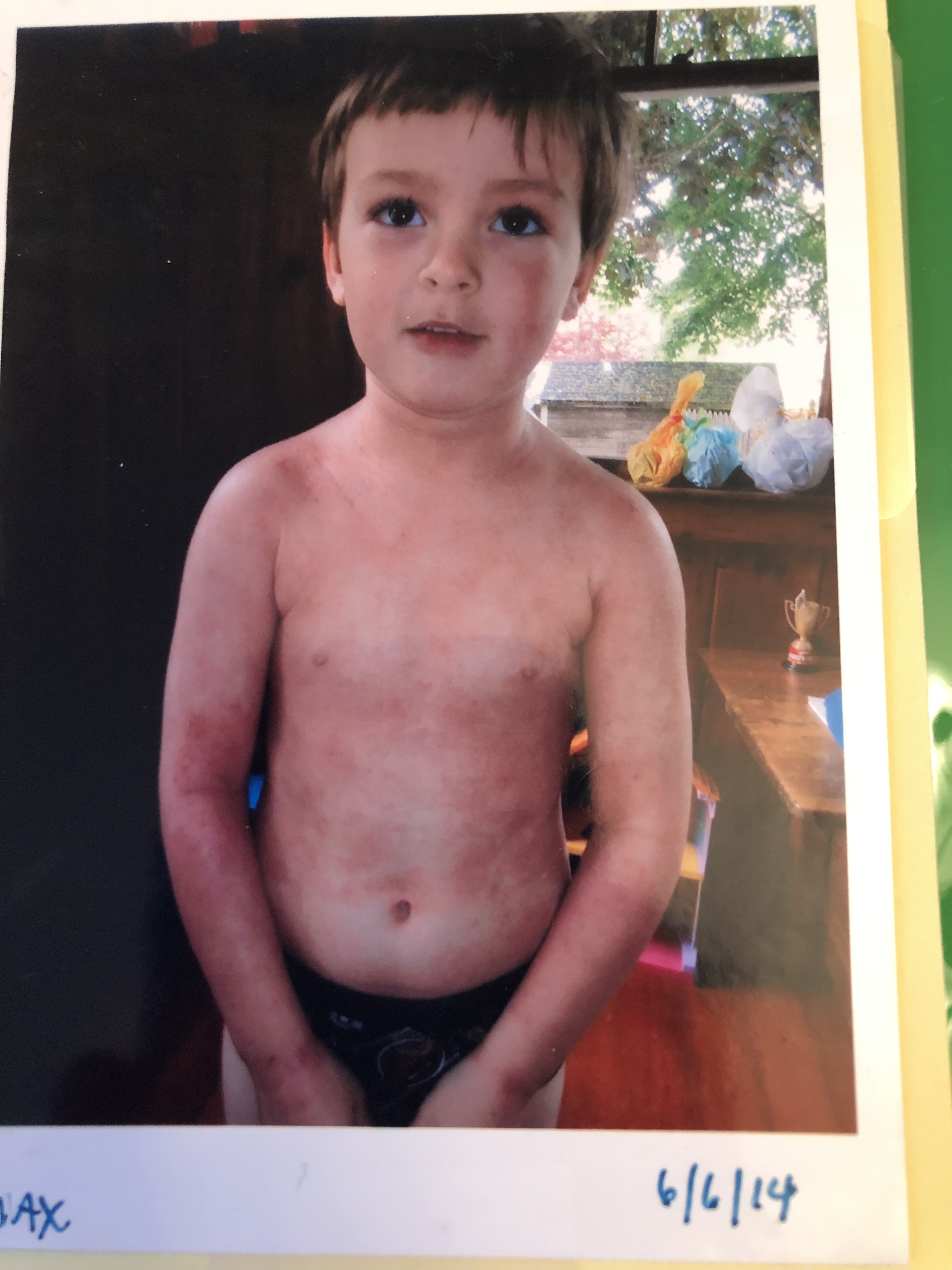

June 2014 (4 yr 7 mo) – 6/1 – Max stopped all topical steroid creams. He developed Red Skin Syndrome also known as Topical Steroid Withdrawal Syndrome, as his skin had become addicted to the synthetic cortisol in the creams. His blood vessels were no longer being suppressed by the creams and it is said by others in recovery that blood vessels can dilate up to 3x the normal size off the creams, causing terrible nerve pain and itch. His back flared first with rashes and gradually healed. The skin on his knees turned gray and thick for weeks, resembling elephant skin.


November 2014 (5 yrs) – Max’s face flared with rashes, shedding and weeping skin for over 6 months. He experienced ongoing nerve pain and itch. He saw medical providers weekly throughout his early years in TSW, and was treated with everything from compounded antihistamines, to supplements, vitamins, a compounded antibiotic, genetic testing, comprehensive lab work including allergy testing and more. Ultimately comfort measures from ice packs to sunlight, sleeping at whatever time of day was possible, and allowing the nonlinear progression of healing to lead the way brought recovery.



April – August 2015 (5 yr 5 mo) – Ongoing rashes body wide, nerve pain and itch.
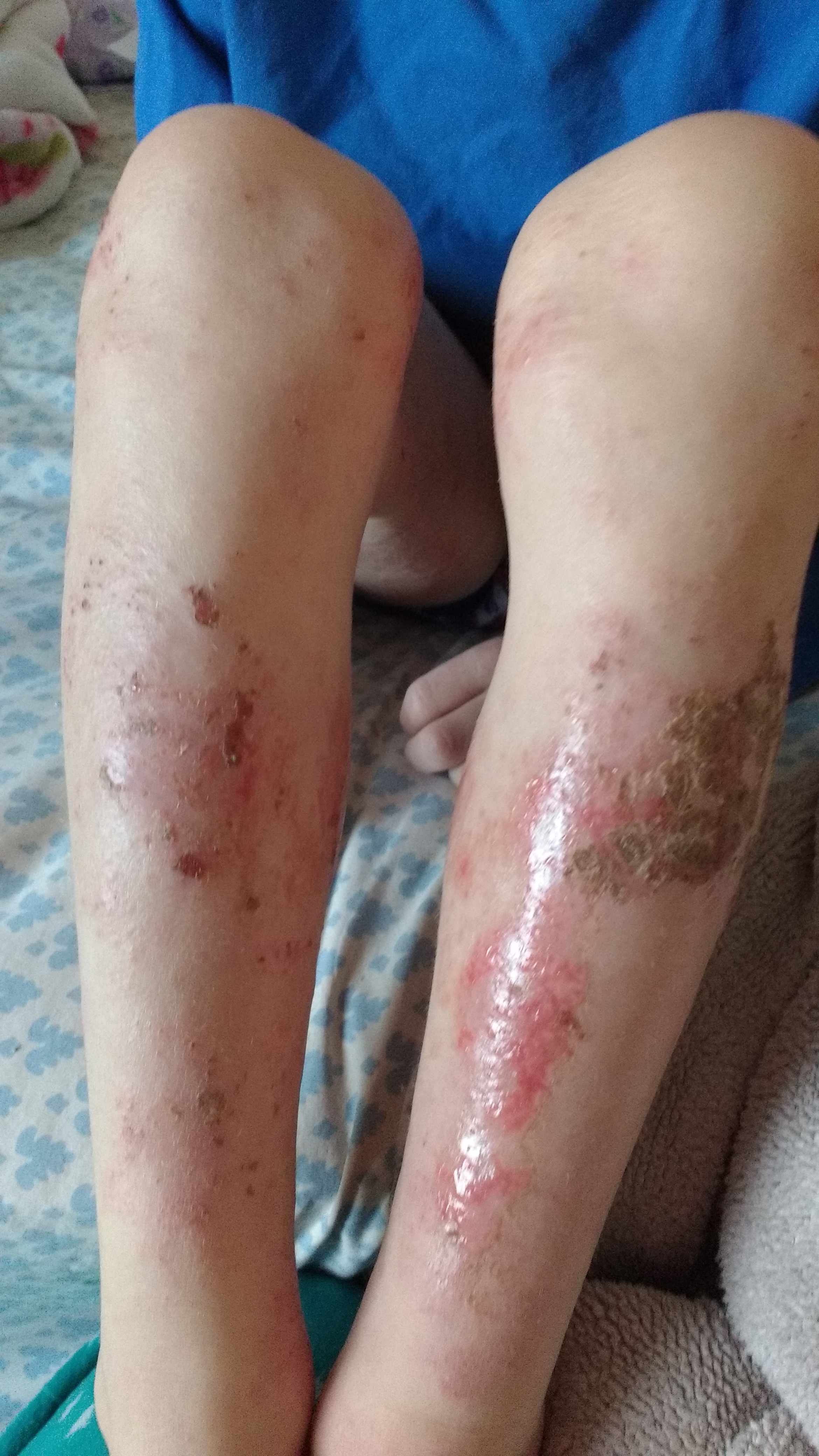

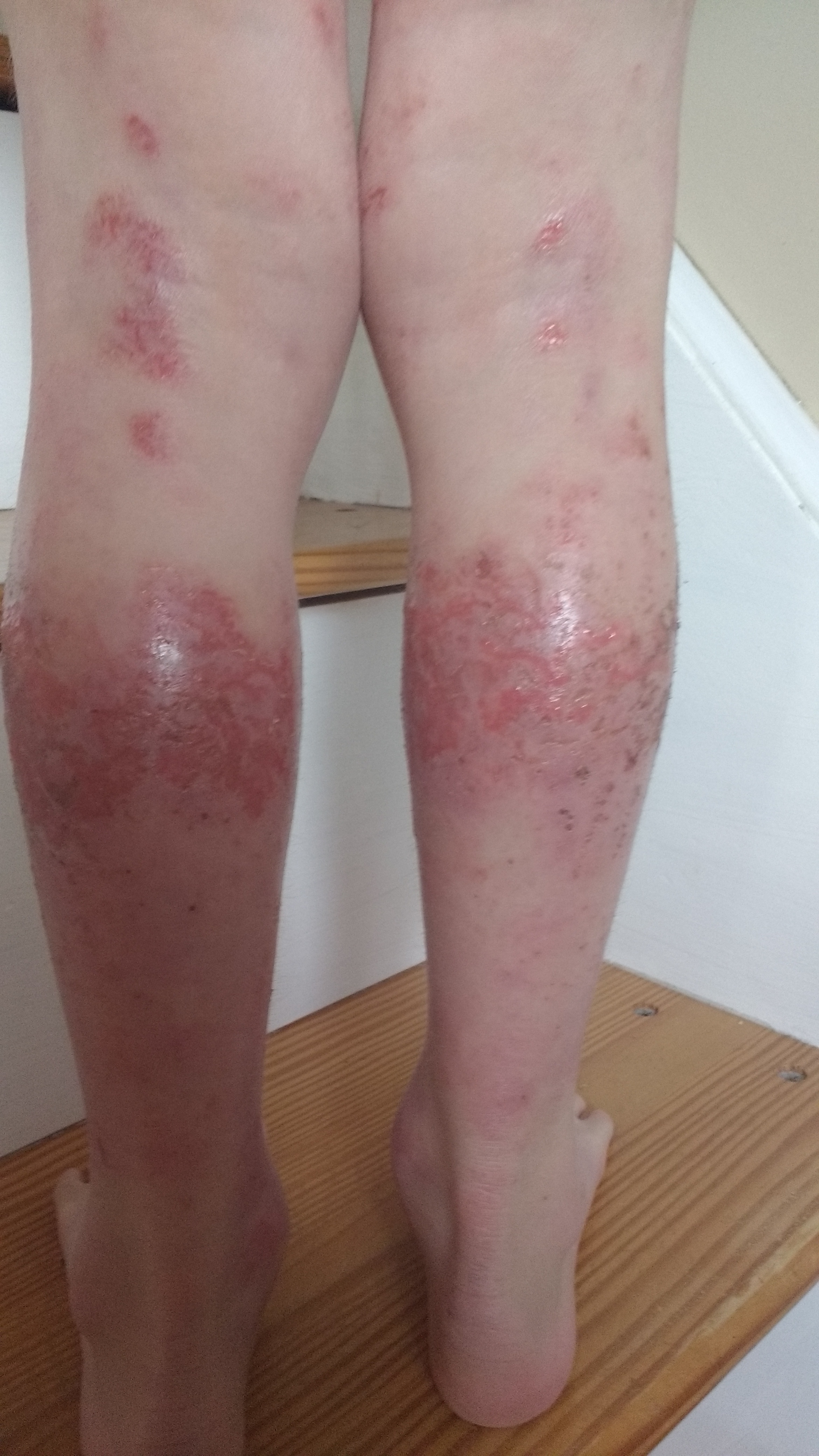

February 2016 (6 yr 3 mo) – Ongoing rashes body wide. Weeping skin. Ongoing nerve pain and itch. Fourth picture is March 2016, less weepy.
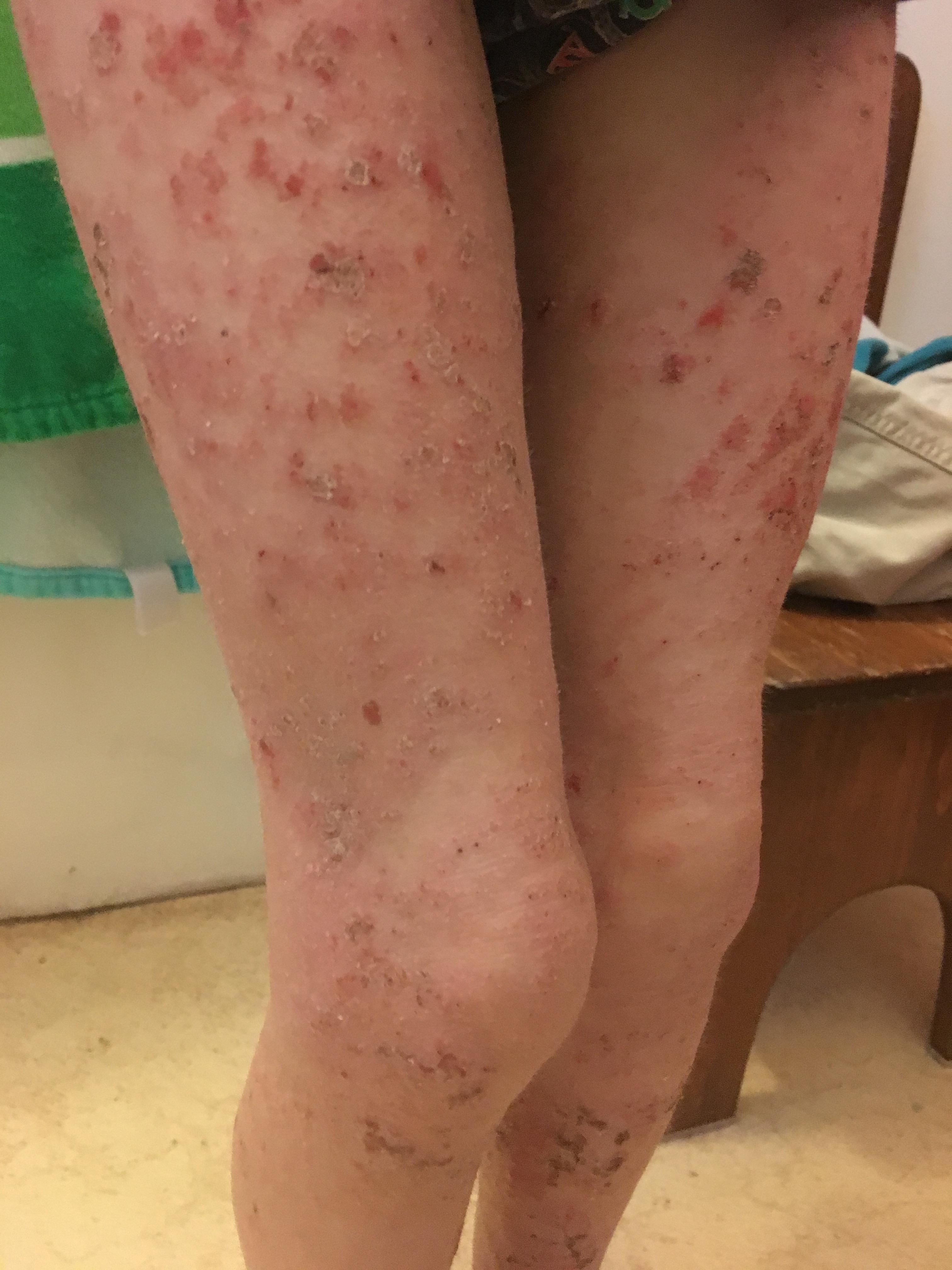
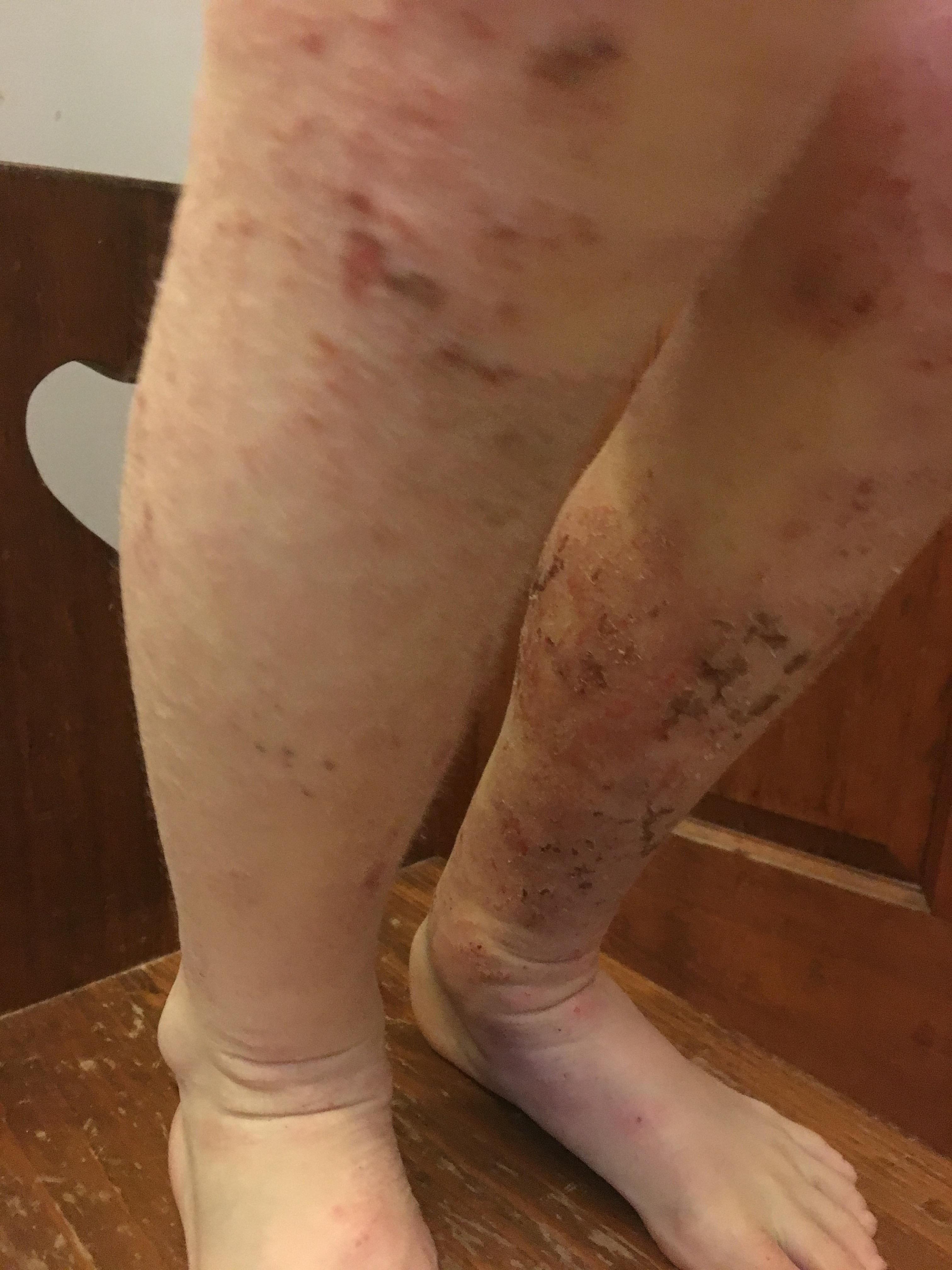
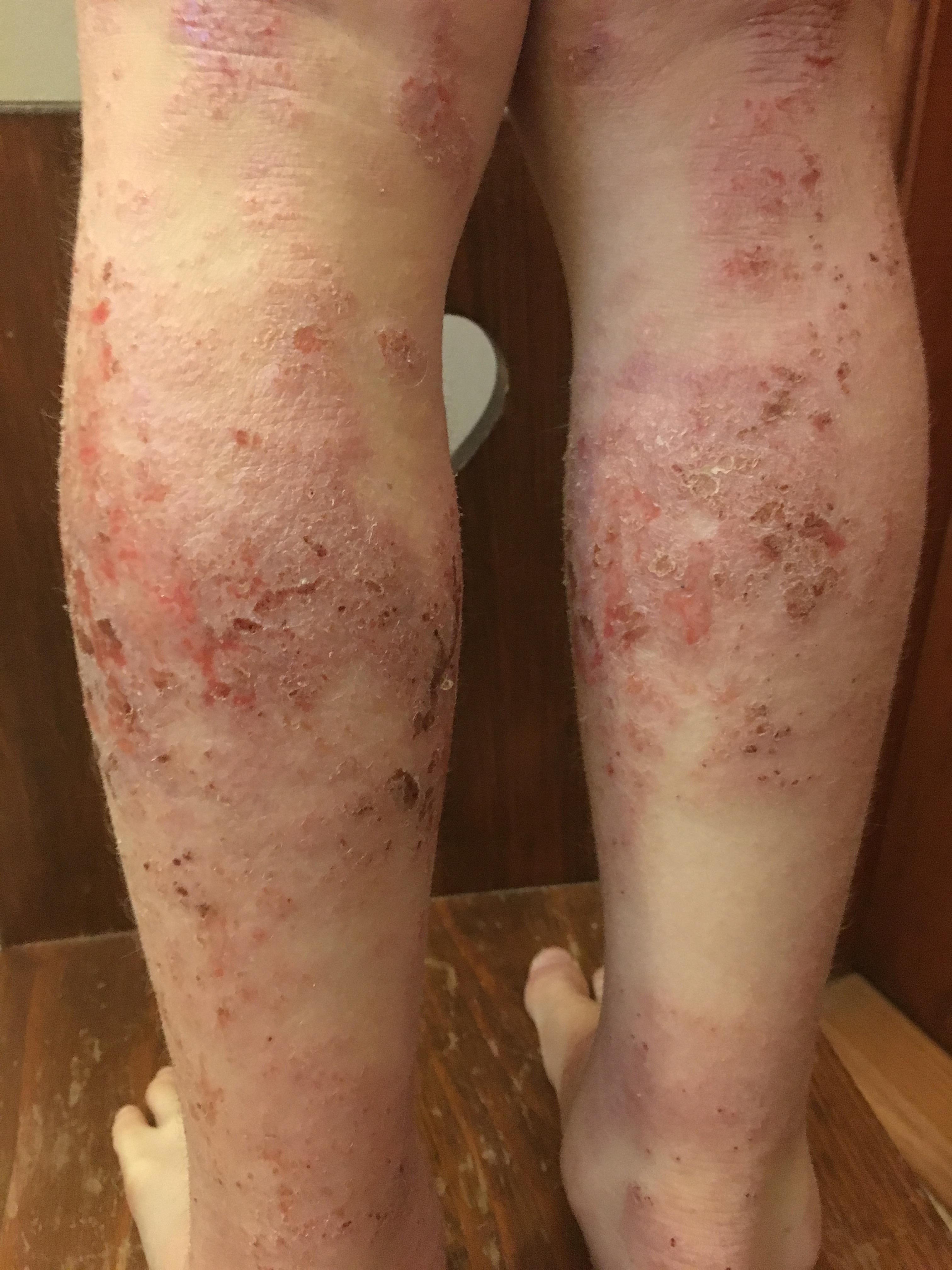
March 2017 (7 yr 4 mo) – Ongoing rashes body wide. Ongoing nerve pain and itch. Ongoing sleep and temperature dysregulation.
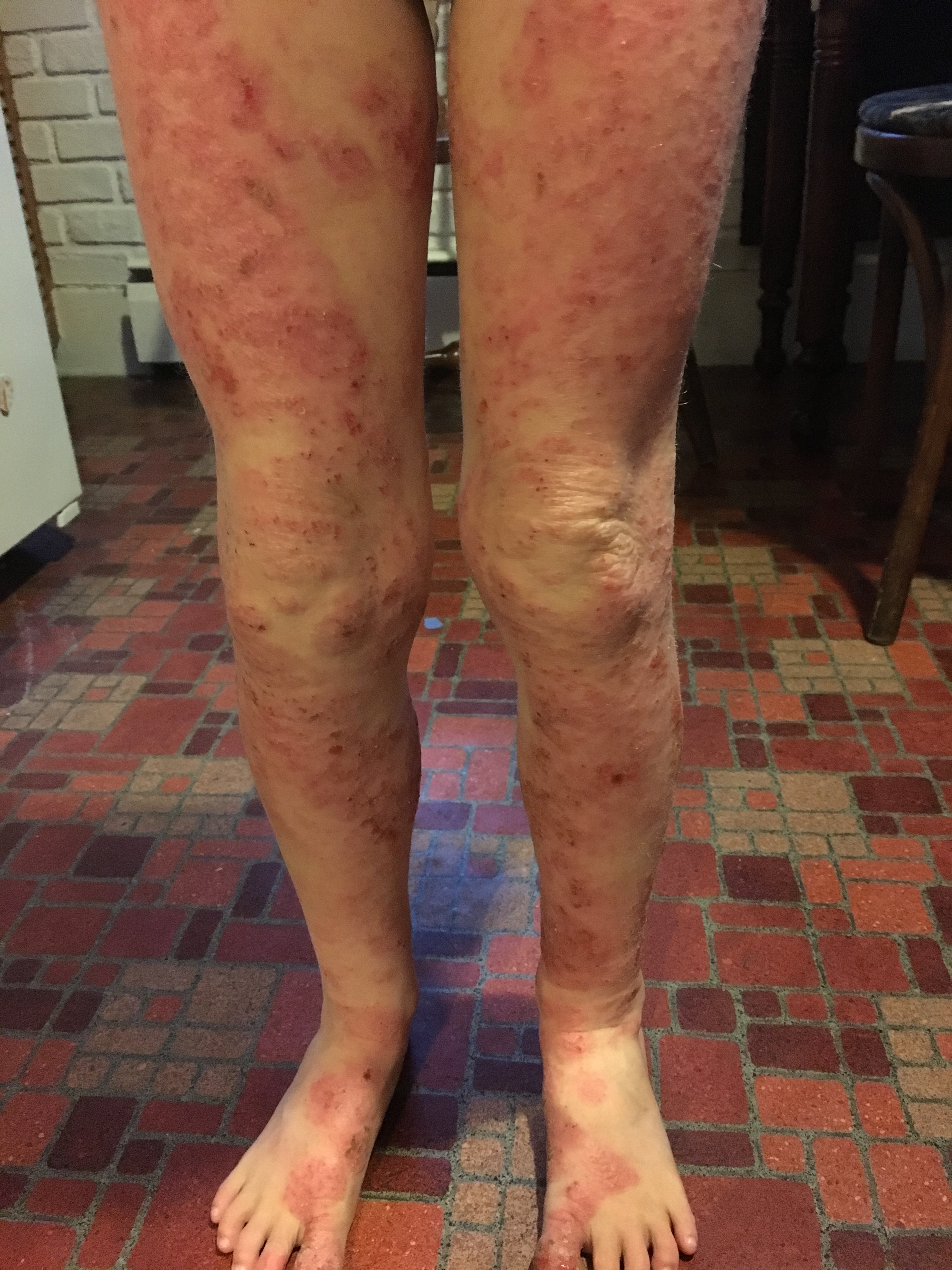
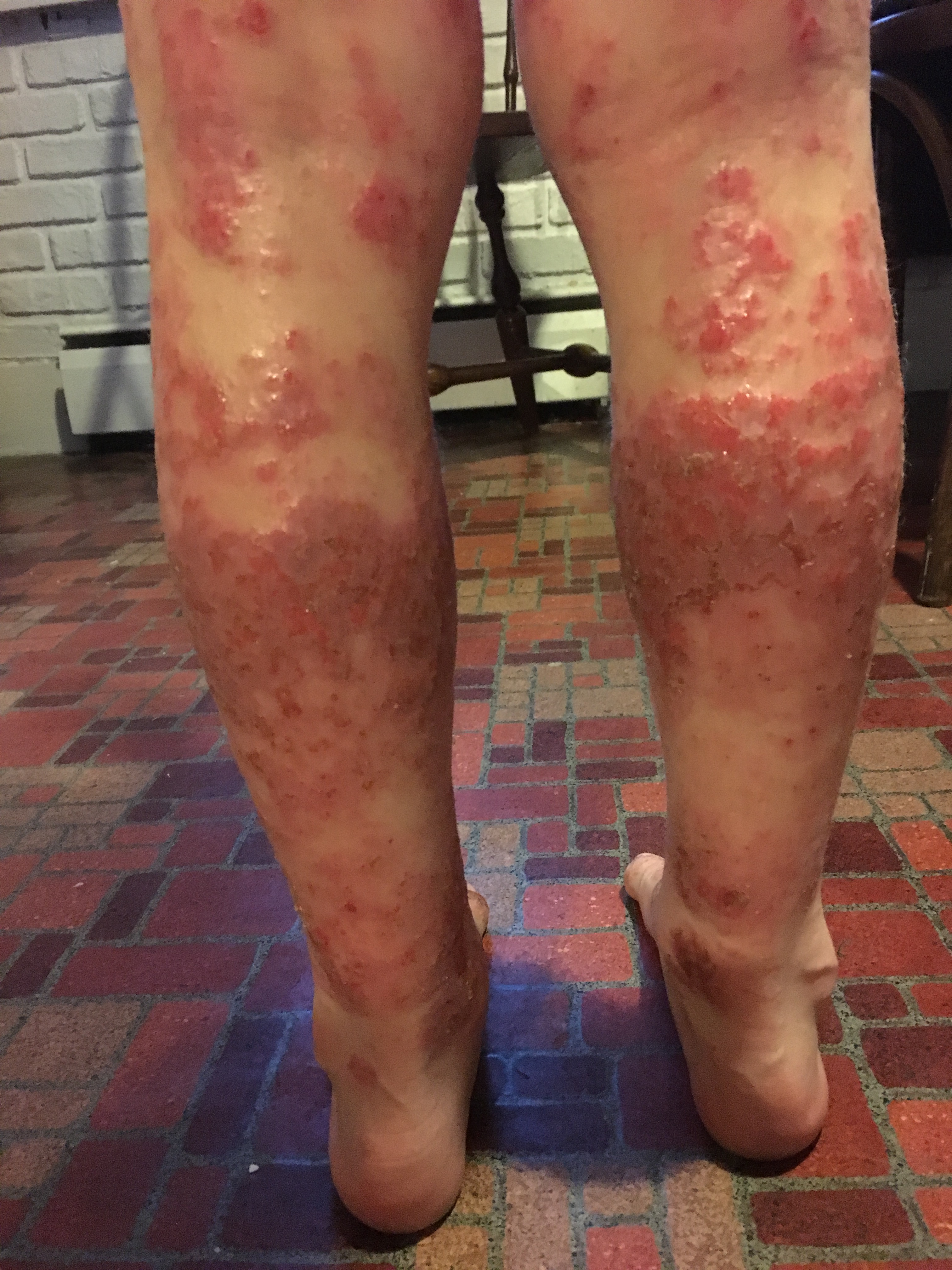
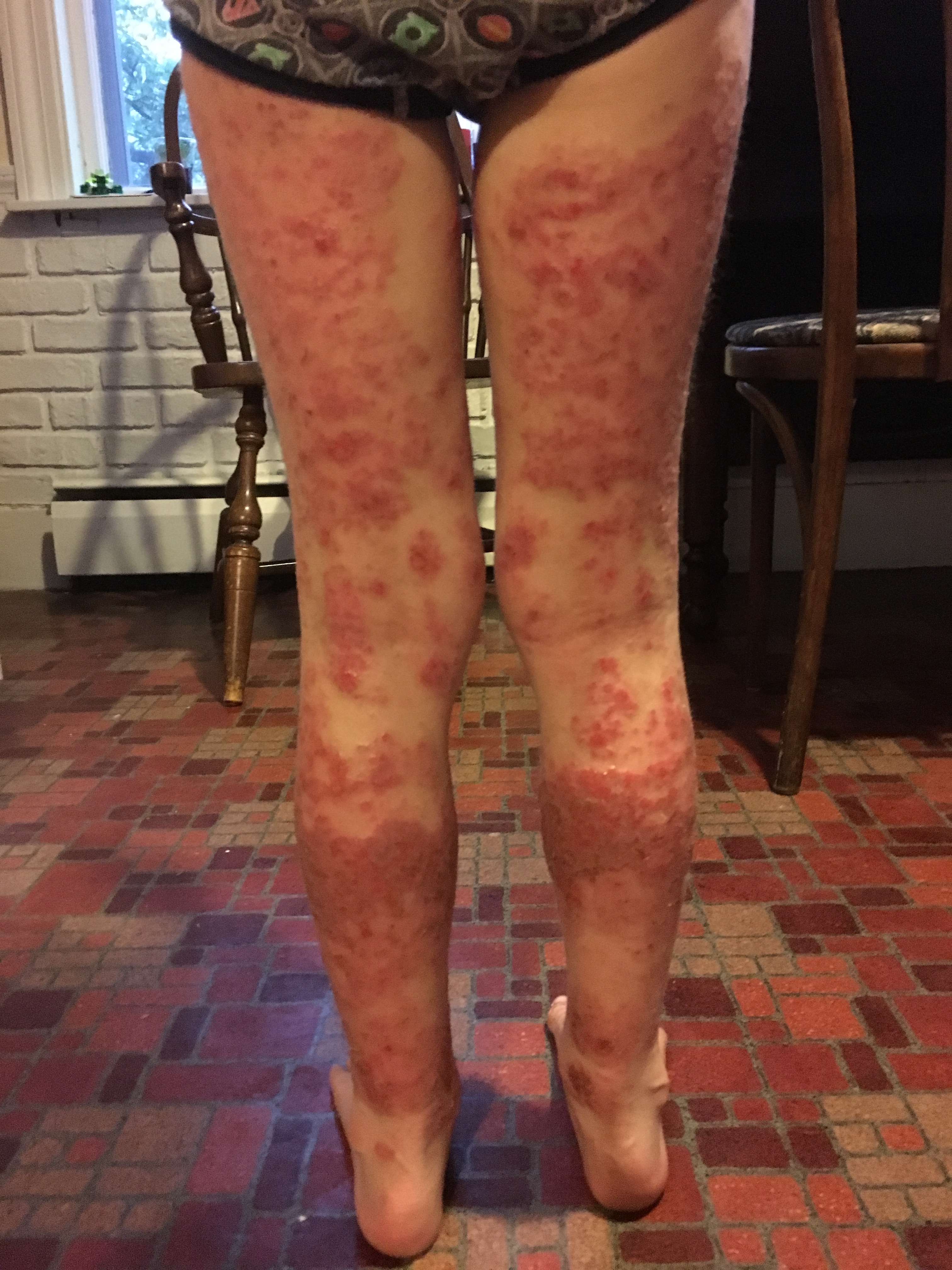
August 2017 (7 yr 9 mo) – Worsened, steroid induced red rashes. In May 2017 Max developed a respiratory issue. He was hospitalized and his treatment included a 3 day course of oral steroids and a 2 week course of a steroid inhaler. He developed side effects to both and by the second week could only tolerate a half a dose of the steroid inhaler. Two days after stopping the steroid inhaler, at the time of day his body was used to it being administered, Max had a severe rebound with sudden neck swelling. In the above pictures Max’s skin presents similar to medical photos of individuals experiencing a drug allergy. His skin may have been additionally irritated following a two week dose of a compounded thyroid hormone when a pediatric endocrinologist failed to recognize and support the signs of rebound to a steroid inhaler.
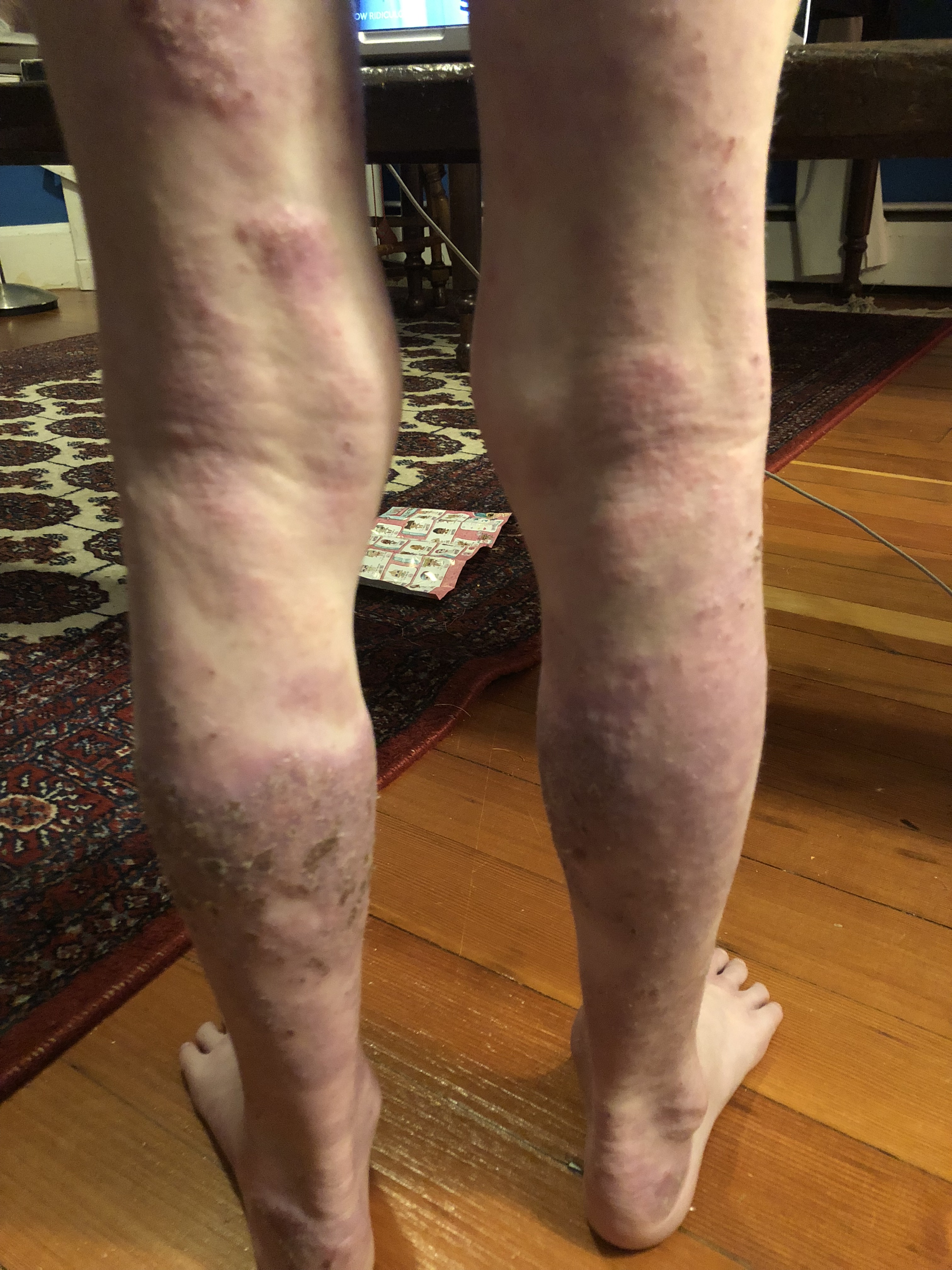

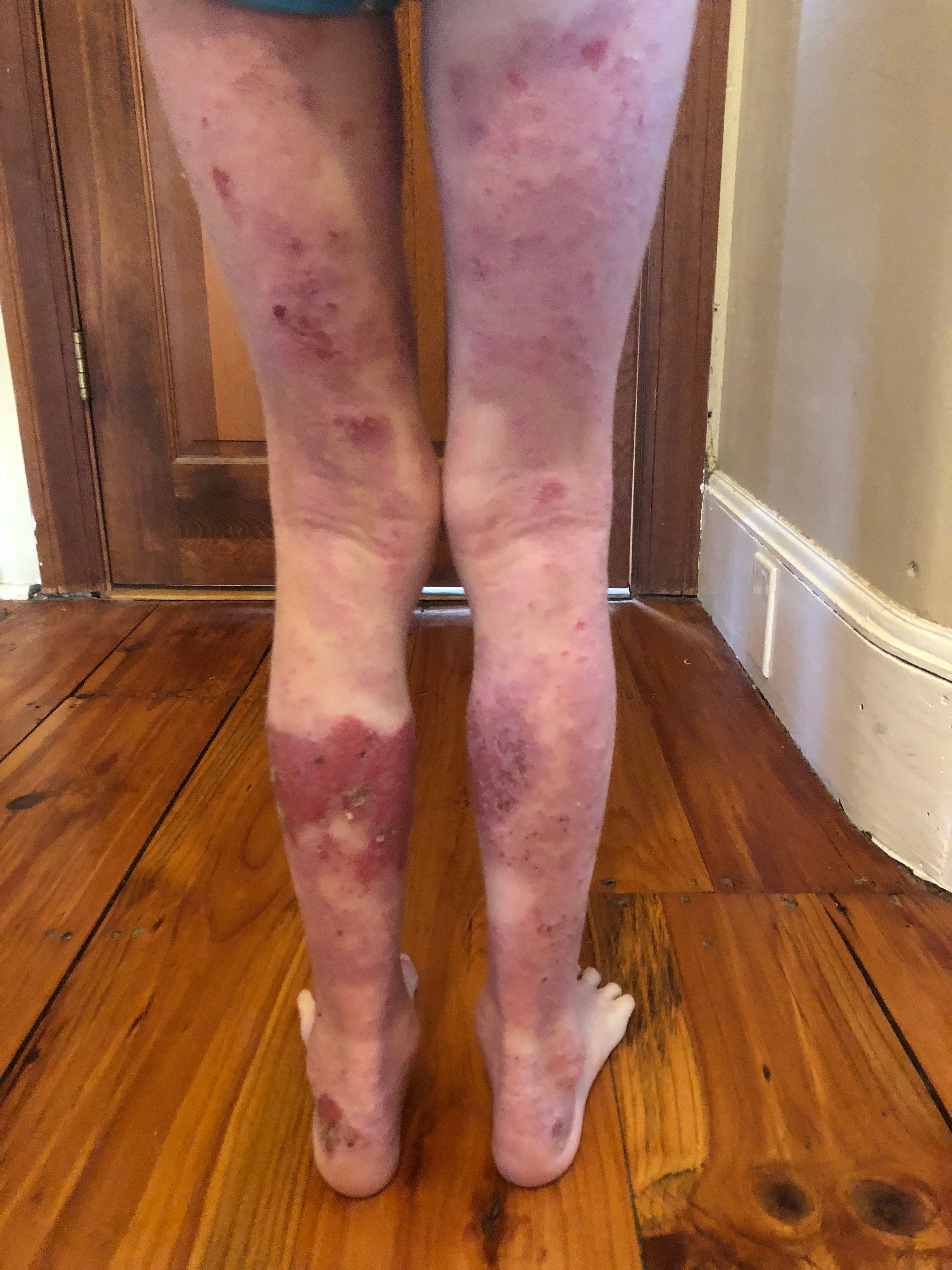
November 2018 (9 yr) – Stages of healing and flaring on back of calves. Ongoing rashes, nerve pain and itch.
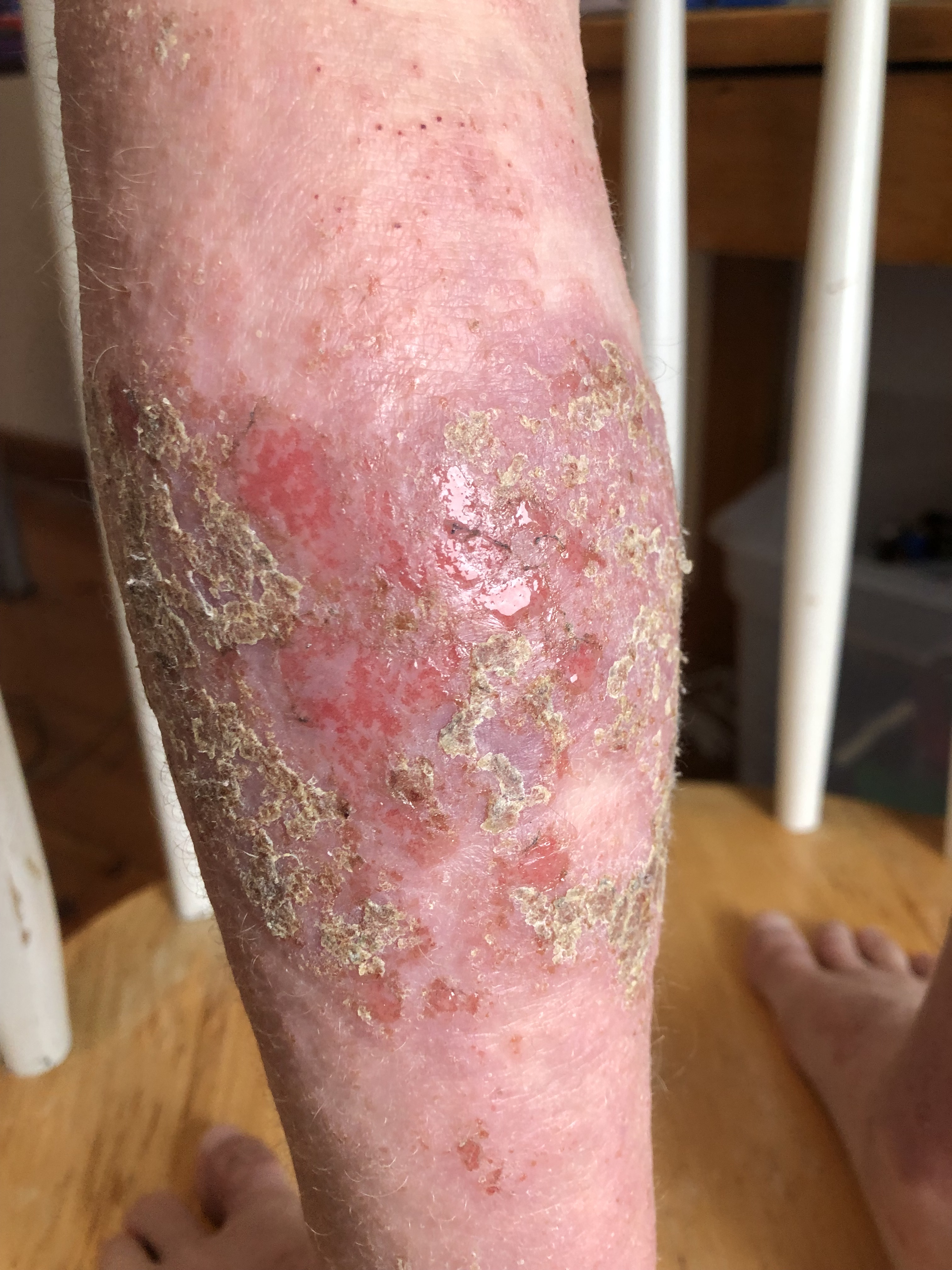
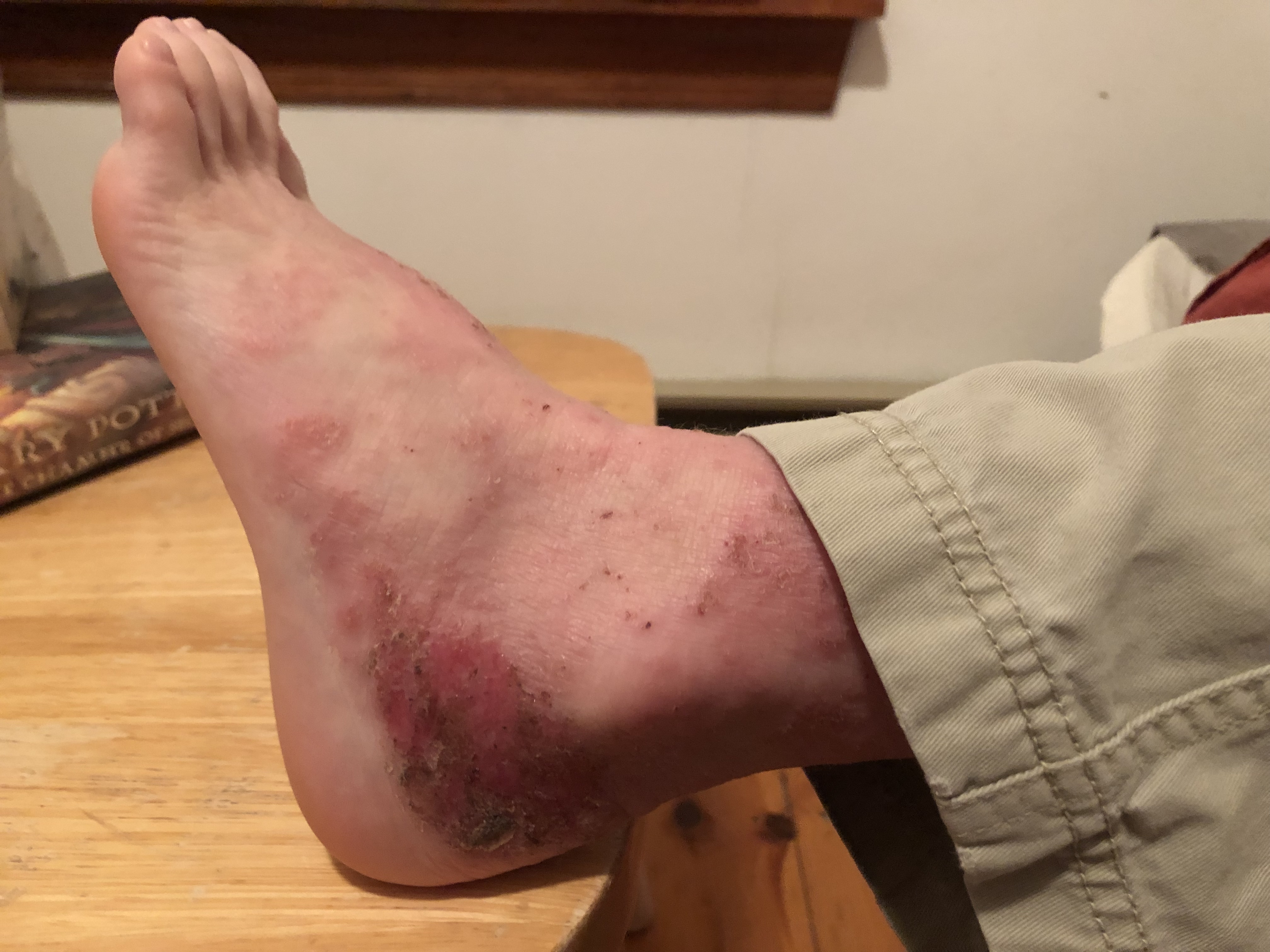


January – February 2019 (9 yr 2 mo) – Stages of healing and scabbing on back of calves. Max stopped wearing sneakers in gym this month to allow for wounds on his heels to develop and maintain scabs.


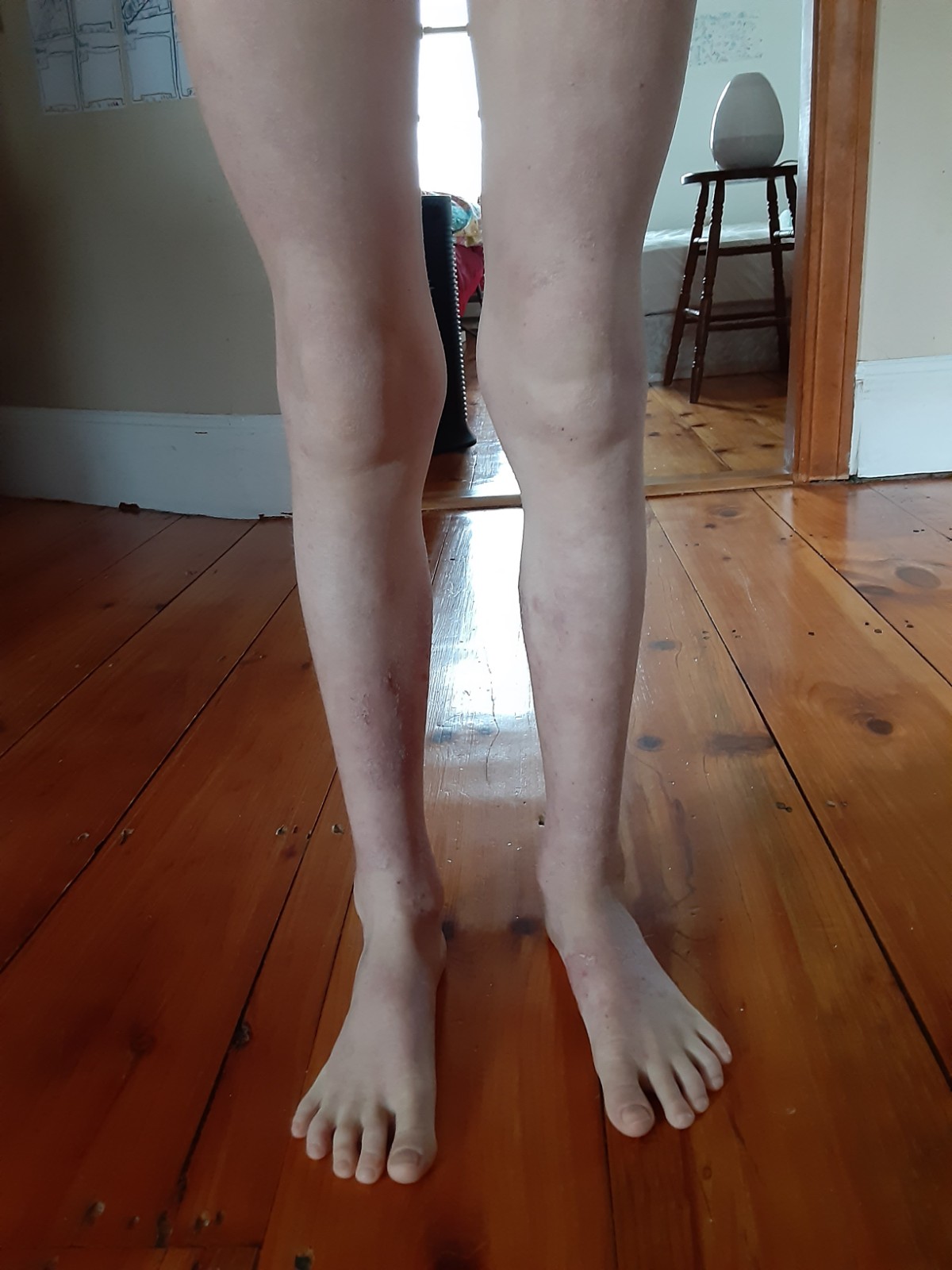
February 2020 (10 yr 3 mo) – Max still has areas of healing on his calves that are slower to heal as they are impacted by the joys of running and playing sports. He has almost no itch or nerve pain during the day. He sleeps more deeply at night than before but still experiences nerve pain and itch as the last areas of skin recover. (Update at age 11 years old, all nerve pain and itch has resolved).
Topical Steroid Withdrawal Syndrome, a result of ineffective and mismanaged topical steroid cream treatment, worsens the original health issue at a magnitude of suffering and pain greater than can ever be explained in pictures or words. Current gaps in topical steroid cream treatment, from lack of a trackable dose, to the need for safe monitoring of symptoms, puts patients at risk. Improved labeling on topical steroid creams to warn about the potential adverse effect of Topical Steroid Withdrawal Syndrome is critical. Share our story and be part of stopping Topical Steroid Withdrawal Syndrome. Every. Provider. Will. Know.
Jolene MacDonald
jmacdonald@itsan.org